Sign up for the daily CJR newsletter.
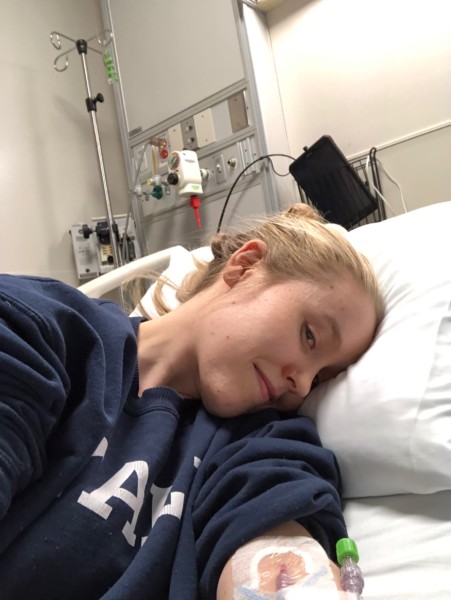
On March 3, I watched developing coverage of the first confirmed case of community-spread covid-19 in New York City. Ten days later I began to show symptoms of covid-19. I was hospitalized.
In the past five months I’ve gone from journalist to patient to interview subject and back again. Along the way, I gained important insights about the ways journalists cover and interact with covid-19 patients.
When I tested positive for the virus, on March 17, I began sharing my story on Instagram. A few days after being discharged from the hospital, I shared my full account in a New York Times op-ed. I soon heard from CNN, NBC, and BuzzFeed, among other outlets, and I began connecting with covid-19 patients all over the world. In late March, I launched the Body Politic covid-19 Support Group with a colleague, friend, and fellow patient, which now provides resources and emotional support to thousands of people with covid-19.
In March and April, most stories about covid-19 patients focused on those with respiratory symptoms, particularly those who were on ventilators. While I too had been hospitalized for shortness of breath, I did not require intubation, though for a month after returning home I still struggled with a wide range of symptoms. Thanks to further medical research, and the efforts of journalists committed to understanding the diversity of covid-19 patient experiences, we now understand that the virus can affect nearly every system of the body, and that there are “long haul” patients, who remain sick for weeks and months after their initial symptom onset. But mainstream news coverage still tends to ignore some important issues, like patients’ mental health, medical bias, testing issues, and symptom relapse.
As media inquiries came in for my support group, I began to work as a liaison between the press and covid-19 patients, eventually setting up a free media training with glaad. As other patients followed a similar media trajectory to mine, posting viral tweet threads, appearing on CNN, and sometimes writing op-eds of their own, we traded both advice and warnings.
While many covid-19 patients deal with debilitating fatigue, many journalists seem unaware of this symptom and its impact on patients’ lives. After I was discharged from the hospital, I experienced daily fatigue, accompanied by splitting headaches and eye pain. Researchers have since drawn links between long-haul covid-19 symptoms and myalgic encephalomyelitis (ME), a complex chronic disease. People with ME and those who treat them often advocate for “pacing,” an energy-management technique that many covid-19 patients also utilize. During a recent BBC interview in which I appeared alongside Paul Garner, a tropical-disease specialist and covid-19 patient in my support group, Garner described needing to schedule rest before the interview in order to participate.
Lauren Nichols, a thirty-two-year-old long-haul patient in Boston, finds “spoon theory,” a tactic similar to pacing, helpful in regulating her energy. Nichols says many reporters don’t understand that she’s conserving energy. She commends those who reach out in advance via email and warns against last-minute attempts to interview patients. “You can’t do that to someone who’s dealing with symptoms,” Nichols said. “I might be on the toilet for the next four hours!”
David Lat, who received early and frequent media attention after being placed on a ventilator in New York City at age forty-four, also recounts working around his symptoms while conducting interviews. “My voice was pretty bad because of damage on my vocal cords from the ventilators,” Lat said; he conducted one interview via direct messages on Twitter. Nichols also often prefers written interviews, explaining that “there were…many times when I didn’t have the energy to verbally communicate, but I did have the energy to write an email.” Respecting patients’ time, understanding that some may need to cancel or reschedule appearances, and offering multiple methods of interviewing are helpful ways reporters can gain trust and facilitate successful interviews.
Journalists must also carefully navigate patient privacy. Lat, Nichols, and I shared our stories because we wanted to raise awareness and demystify a confusing and frightening disease. But the media attention that results from going public with your experience can become overwhelming. I still receive daily media requests as well as comments, DMs, and emails from people who have seen me on the news or read my stories. While the majority of these communications are supportive, I’ve also been the target of trolling and digging in to my personal medical history. Nichols recently refused what she considered an invasive request from a reporter who asked to be connected with her doctor to fact-check her symptoms and positive test result. While fact-checking is important, hipaa prevents doctors from providing such information without patients’ consent, and journalists will benefit from a more sensitive approach when working with patients who may have experienced medical gaslighting.
Journalists should also be aware that some patients never test positive for the virus. Tests are still hard to access and results are often massively delayed. Nichols, Lat, and I all tested positive for covid-19, but we were lucky. When I was finally tested in New York City in March, it was after repeated attempts and denials. The person who infected me was never able to receive a test, and Lat recounts similarly struggling to get tested. There are also reliability issues for diagnostic covid-19 tests, which is why some doctors, scientists, and health officials don’t rely on them—so why do journalists?
I have argued before that covid-19 testing is a social justice issue, because many of the groups most affected by test accessibility are already marginalized. When reporters focus only on patients who have received a positive covid-19 test, they risk excluding those whose stories don’t neatly fit the mainstream narrative, and promoting a patient experience that is overwhelmingly economically privileged.
Interviewing patients with diverse test results doesn’t mean reporters have to ignore those results or the fact that some patients may have trouble confirming whether their symptoms are covid-related. In fact, including patients who have tested negative, received inconclusive results, or were unable to be tested at all provides an opportunity for journalists to discuss the reliability and accessibility issues of covid-19 tests, as well as the confusion many doctors face when diagnosing this virus. Science writer Ed Yong successfully navigated this issue in a recent piece in The Atlantic on long-haul covid-19 patients. The reliability issues around testing and diagnosing covid-19 are important and under-discussed aspects of the current pandemic that I believe should be at least briefly mentioned in any piece of journalism on covid-19 patients, as false positive results can also occur.
When interviewing covid-19 patients, awareness about the language patients use to describe their experiences can help reporters ask relevant questions. The question of whether a patient has “recovered,” for example, ignores the complexities of the covid-19 experience. For example, Nichols says she’s technically considered recovered by the commonwealth of Massachusetts, because she no longer tests positive for the virus, but she is still experiencing persistent and debilitating symptoms.
Lat recently wrote an op-ed in the LA Times arguing that “recovering from a severe case of covid-19 is not like switching a light on or off. It’s more like a dimmer switch, where the light gets brighter, then darker, then brighter again.” Like me, Lat recounts continually being asked whether he’d recovered after his discharge from the hospital, and told me he still doesn’t “really know.” The fact that some patients experience fleeting recoveries only to relapse into old symptoms also makes many hesitant to publicly announce their recovery. Reporters looking to understand a patient’s progress might ask whether the patient is still experiencing any symptoms of the virus, or about long-term physical, mental, or financial effects.
The question of recovery is connected to another controversial but commonly used word: “survivor.” While many covid-19 patients seem to like the word “survivor,” others feel it leaves out long-haul patients who have not yet survived the virus, and is inappropriate given the many issues patients deal with after recovery. Nichols says she’s come to “hate” the word. “I don’t know if I’m a survivor,” Nichols told me. “I don’t know if two weeks from now I’m going to get a clot that’s going to take me out.” Instead of using the term “survivor,” when writing about patients still experiencing effects of the virus, I use the word “patient,” or the phrase “person living with covid-19.” Nichols agrees: “While someone is still symptomatic, referring to them as a patient validates that…you’re still having pain.”
NICHOLS, LAT, AND I all shared our stories because we wanted to raise awareness and demystify the terrifying experience of contracting covid-19. We came to the arena with varying levels of media experience—Lat and I had both worked in journalism, whereas Nichols had never spoken to the press—but we’re all having to learn new boundaries and guidelines as we navigate this novel virus and the best ways to share information about it.
Sharing our stories also helped us find community. Nichols joined my support group after reading one of my articles, and Lat says he likewise connected with patients and their families. “It was really helpful to be able to pay it forward, and to be able to pray for other people, as I was prayed for,” Lat explained.
As Nichols, Lat, and I all discovered, covid-19 patients aren’t just participants in media coverage, they’re also often big consumers of covid-19 related news. As journalists writing about the disease, we must be aware that our work may be received by two very different audiences—patients who are often educated about their illness and sensitive to certain reporting approaches, and members of the general public who don’t understand the intimate experience of contracting the virus.
Bridging this gap isn’t easy—especially during a fast-moving pandemic, when knowledge is constantly shifting—and may require a rethinking of deadlines and newsroom policies, but it is both possible and necessary.
NEW AT CJR: When the news becomes religion
Correction: An earlier version of this post misstated David Lat’s age when he was placed on a ventilator. He was forty-four, not forty-five.
Has America ever needed a media defender more than now? Help us by joining CJR today.